🎯 Quick Answer
What: Healthcare process improvement applies systematic methodologies like Lean Six Sigma to reduce variation, eliminate waste, and improve patient safety across clinical departments from operating rooms to emergency departments.
Why It Matters: Hospitals implementing healthcare quality improvement programs achieve 30-40% reductions in medical errors, 20-35% decreases in patient wait times, and measurable improvements in clinical outcomes and patient satisfaction.
How to Apply: Deploy DMAIC methodology across patient journeys, implement statistical process control for clinical metrics, and engage frontline staff in continuous improvement focused on patient safety.
Expected Results: Most healthcare systems see 25-40% reduction in preventable harm events, 15-30% improvement in patient flow, and significant gains in Leapfrog grades and CMS star ratings within 18-24 months.
The 3 AM Decision Point
An experienced OR nurse watches the monitor. The patient's vitals show subtle changes. Textbook normal ranges. But the pattern feels wrong.
She calls the surgeon back. He's annoyed. "Numbers are fine," he says. She persists. He returns.
They find a slow bleed the monitors hadn't flagged yet. Another hour and the patient would have coded.
Down the hall in the ER, a similar pattern unfolds. A triage nurse notices breathing rhythm changes before oxygen saturation drops. Early intervention prevents ICU admission.
Two departments. Same principle. Different outcomes based on whether the system amplifies or ignores pattern recognition.
The Healthcare Quality Gap
Healthcare faces a paradox. The industry employs brilliant clinicians using cutting-edge technology, yet systems fail patients 250,000 times annually through preventable medical errors.
The gap isn't clinical knowledge. It's process excellence.
After implementing healthcare process improvement across multiple hospital systems, the pattern becomes clear. Excellence in healthcare requires both clinical expertise and systematic operational discipline.
What Healthcare Process Improvement Really Means
Healthcare quality improvement goes beyond fixing individual problems. It creates systems where excellence becomes the default, not the exception.
The Three Process Layers
Clinical Processes:
Surgical protocols and checklists
Medication administration workflows
Diagnostic pathways and decision trees
Treatment protocols and care plans
Operational Processes:
Patient flow from admission to discharge
OR scheduling and turnover efficiency
Supply chain and inventory management
Bed management and capacity planning
Support Processes:
Lab result turnaround times
Pharmacy fulfillment speed
Transport and logistics coordination
Communication and handoff protocols
💡 Critical Insight: Patient safety improves when all three process layers work in harmony. Most healthcare quality improvement efforts focus only on clinical processes, missing 60% of the opportunity.
The OR to ER Journey
Following a patient's journey reveals where healthcare process improvement creates the greatest impact.
Operating Room Excellence
The Challenge:
First case delays cascade through the day
Turnover times vary 40-60% between cases
Supply availability unpredictable
Communication gaps during handoffs
The Process Improvement Approach: Healthcare systems applying Lean methodology to OR operations see remarkable results.
A 400-bed regional hospital reduced first case start delays from 45% to 8% within six months. The approach focused on standard work, not individual performance.
Key Changes:
Standardized pre-op preparation sequences
Visual management boards for supply status
Statistical process control for turnover times
Structured handoff protocols between shifts
Results:
30% increase in OR utilization
25% reduction in overtime costs
40% improvement in surgeon satisfaction
Zero preventable delays in 90 days
This mirrors patterns from semiconductor manufacturing, where yield optimization requires controlling every variable in the process, not just the obvious ones.
Post-Operative Care Transitions
The handoff from OR to recovery represents a critical patient safety vulnerability.
Traditional Approach: Verbal communication. Rushed transitions. Missing context. Assumptions about what matters.
Improved Protocol: Structured handoff checklist borrowed from offshore oil rig shift changes. Every critical parameter confirmed. Every concern documented. Every question answered before transfer.
Healthcare organizations implementing structured handoffs see 35-50% reduction in post-operative complications from communication failures.
ICU Process Excellence
The Flow Problem: ICUs face constant capacity constraints. Delayed discharges create bottlenecks. ER holds accumulate. Elective surgeries get cancelled.
The Healthcare Process Improvement Solution: A multi-hospital system applied value stream mapping to identify delays. The analysis revealed that clinical decisions weren't the constraint. Process gaps were.
Findings:
40% of discharge delays: waiting for prescriptions
25% of delays: transportation coordination
20% of delays: family communication timing
15% of delays: actual clinical considerations
Process improvements targeting non-clinical delays freed 20% more capacity without adding beds or staff.
Emergency Department Transformation
ERs struggle with unpredictable demand, complex patient needs, and resource constraints.
Common Metrics That Mislead:
Average wait time (hides variation)
Patient satisfaction scores (lag indicators)
Bed occupancy rates (measure capacity, not flow)
Better Healthcare Quality Improvement Metrics:
Door-to-provider time variation (statistical process control)
Left without being seen rates (system failure indicator)
Boarding hours (downstream constraint measure)
Time to disposition decision (process efficiency)
A 600-bed hospital system reduced ER wait times 60% by focusing on variation reduction, not average improvement. The breakthrough came from treating patient flow as a continuous process, not discrete events.
Cross-Industry Pattern Recognition
Healthcare process improvement accelerates when lessons transfer from other high-stakes industries.
From Oil Rigs to Operating Rooms
Shift Handoff Protocols: Offshore platforms developed structured communication methods where missing information causes disasters. The same protocols prevent healthcare handoff failures.
One hospital system adapted oil industry shift change protocols. Post-handoff complications dropped 47% within four months.
From Manufacturing to Medicine
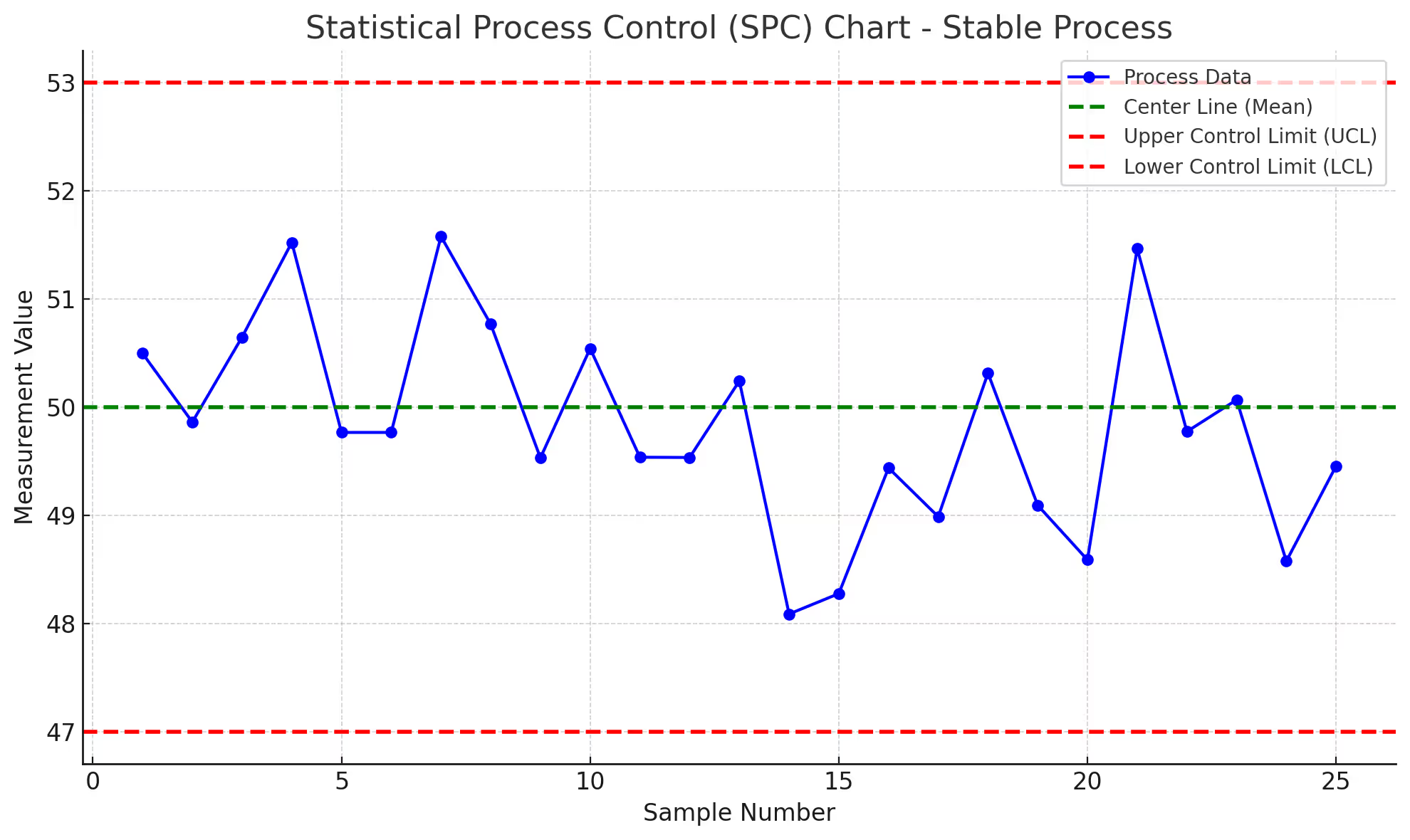
Statistical Process Control Applications: Semiconductor fabs maintain defect rates below 100 parts per million through real-time statistical monitoring. Hospitals applying the same methods to medication administration reduce errors 30-40%.
The Key Difference: Manufacturing focuses on product quality. Healthcare focuses on patient safety. But the statistical principles remain identical.
📊 Data Point: Healthcare organizations applying cross-industry process improvement methods achieve results 40-60% faster than those using only healthcare-specific approaches.
Implementing Healthcare Quality Improvement
Start Small, Think Systems
Phase 1: Baseline Understanding
Map current state patient journeys
Identify variation sources statistically
Engage frontline staff in problem identification
Establish baseline metrics for patient safety
Phase 2: Pilot Implementation
Select high-impact, low-complexity processes
Implement standard work and visual management
Train teams in basic healthcare process improvement tools
Monitor leading indicators daily
Phase 3: Scale and Sustain
Expand to additional departments
Develop Green Belt capability internally
Integrate improvements into workflows
Build continuous improvement culture
Critical Success Factors
Leadership Commitment: Executive support enables resource allocation. Middle management engagement drives implementation. Frontline ownership ensures sustainability.
Data-Driven Decisions: Replace opinions with statistical analysis. Measure outcomes, not just activities. Track variation, not just averages.
Respect for People: Healthcare process improvement succeeds when clinical expertise combines with process discipline. Neither alone produces breakthrough results.
Cross-Functional Collaboration: Patient safety requires coordination across departments. Siloed improvements create local optimization at system expense.
Measuring Healthcare Process Improvement Success
Leading Indicators (Track Weekly)
Near-miss reporting rates (culture measure)
Standard work compliance percentages
Handoff protocol completion rates
Supply availability metrics
Outcome Indicators (Track Monthly)
Patient Safety Indicator (PSI) scores
Readmission rates by diagnosis
Hospital-acquired infection rates
Mortality ratios (risk-adjusted)
System Performance (Track Quarterly)
Leapfrog Hospital Safety Grades
CMS Star Ratings progression
Length of stay variation reduction
Patient satisfaction trend analysis
Frequently Asked Questions
How long does healthcare quality improvement take to show results?
Quick wins appear within 4-8 weeks when focusing on obvious waste elimination. Sustainable culture change requiring statistical thinking and continuous improvement typically takes 12-18 months. Most hospital systems see measurable patient safety improvements within 6 months and significant outcome changes by 12 months.
Can small hospitals implement these methods without extensive resources?
Healthcare process improvement scales to organization size. A 50-bed rural hospital achieved 30% ER wait time reduction using basic value stream mapping and standard work, requiring minimal investment. The key is starting with high-impact processes and building capability incrementally rather than attempting enterprise-wide transformation immediately.
How does healthcare process improvement differ from standard quality programs?
Traditional quality programs often focus on retrospective problem-solving and compliance. Healthcare process improvement emphasizes proactive system design, statistical variation reduction, and continuous improvement culture. It combines clinical excellence with operational discipline, treating patient safety as a systems engineering challenge rather than individual performance issue.
What role do physicians play in process improvement initiatives?
Physician engagement proves critical for healthcare quality improvement success. Early involvement in problem definition, respect for clinical judgment, and data-driven rather than opinion-based discussions increase buy-in. Organizations achieving the best patient safety outcomes create formal physician leadership roles in improvement teams and demonstrate clear connections between process changes and clinical outcomes.
How do you sustain healthcare process improvement gains over time?
Sustainability requires three elements: systematic knowledge transfer (capturing expertise before transitions), statistical process control (detecting degradation early), and continuous improvement culture (making small adjustments routine). Healthcare systems maintaining gains integrate process improvement into operational reviews, tie metrics to leadership accountability, and celebrate progress while addressing variation quickly.
Ready to Transform Healthcare Quality?
🎓 Learn the foundational methodology: Read "What is Lean Six Sigma? The $4.4 Billion Field Reality" to understand the proven framework behind successful healthcare process improvement.
🏥 Explore cross-industry insights: Discover "Cross-Pollination: How Oil Rig Safety Protocols Save Lives in Hospitals" for breakthrough patient safety strategies from high-stakes industries.
Related Reading:
External Resources:
Keywords:
healthcare quality improvement, patient safety, healthcare process improvement, clinical quality metrics, patient flow optimization, medical error reduction, hospital operational excellence, lean healthcare, healthcare lean six sigma, OR efficiency, emergency department improvement, clinical outcomes, quality metrics, Leapfrog grades, CMS stars, PSI indicators, readmission rates, wait time reduction, throughput optimization, DMAIC healthcare, continuous improvement healthcare, cross-industry learning, process excellence, operational discipline
Excellence isn't an event. It's a system. Build processes that protect patients, and performance follows.
Transform healthcare quality through systematic process improvement.